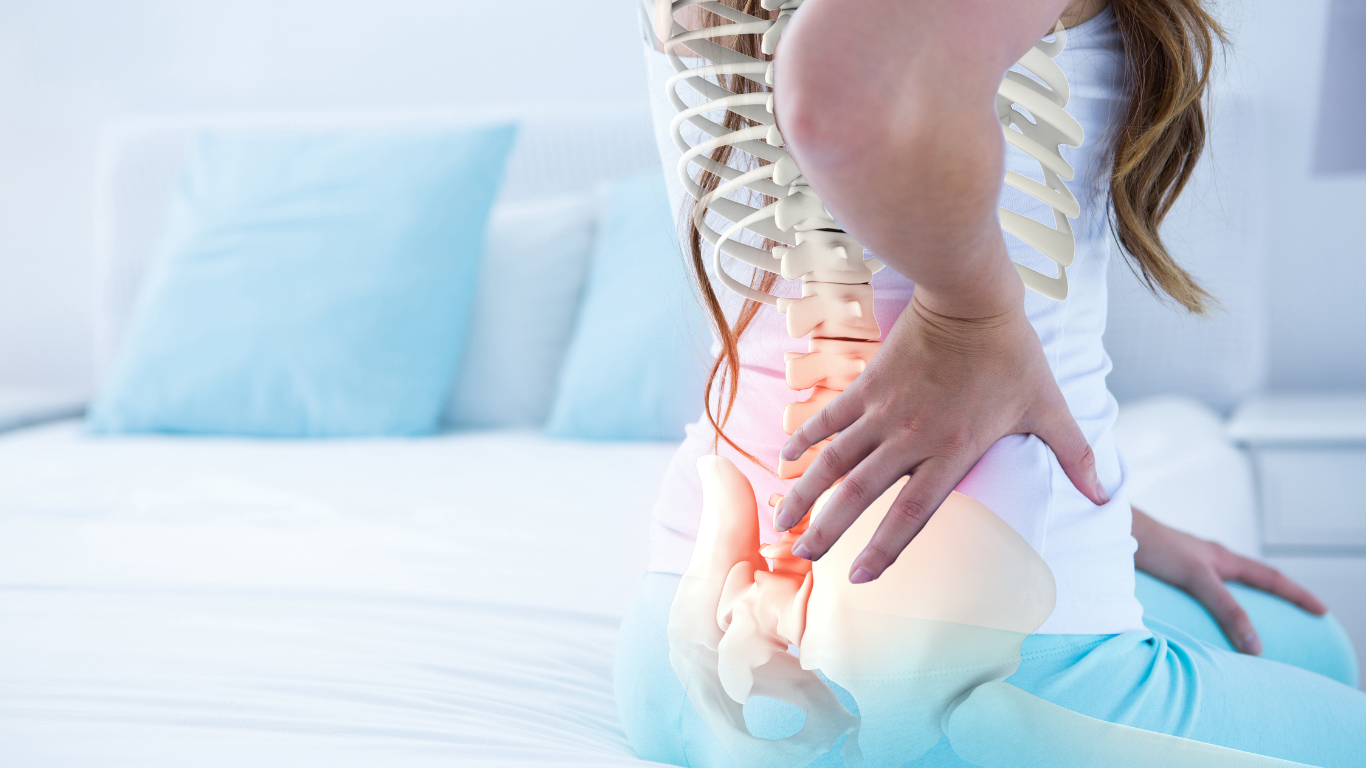
Back pain can feel like a normal part of modern life. Long hours sitting, lifting something the wrong way, or simply getting older can all lead to aches that come and go. But sometimes the pain is different. It travels down the leg, burns, tingles, or causes weakness that makes everyday movement harder.
For many people, these unusual sensations are the first sciatica symptoms, a condition caused by irritation or compression of the sciatic nerve. Because the sciatic nerve runs from the lower spine through the hips and down each leg, even small changes in the spine can trigger powerful nerve pain that affects daily life.
Ignoring these early signals can allow nerve irritation to worsen over time. What begins as mild discomfort may develop into persistent pain, numbness, or muscle weakness that interferes with walking, sleeping, and working.
That’s why recognizing the warning signs early matters. Orthopedic specialists like Dr. Gerardo Mangino, known for compassionate, patient-centered orthopedic care, emphasize that early evaluation often prevents long-term nerve damage and helps patients return to active, pain-free living sooner.
Understanding Sciatica and Why Symptoms Appear
Sciatica is not a disease itself but a symptom of nerve compression or irritation in the lower spine. The sciatic nerve is the largest nerve in the body, formed from several nerve roots in the lumbar spine. When these roots become compressed, inflamed, or irritated, pain and neurological symptoms travel along the nerve pathway.
The condition most often develops when a structure in the lower back presses on the nerve root. This can include a herniated disc, spinal narrowing, bone spur, or inflammation around the nerve.
While occasional back discomfort is common, sciatica symptoms typically follow a recognizable pattern, traveling from the lower back through the buttock and down one leg. Understanding these patterns helps identify the condition early and seek appropriate care before nerve irritation worsens.
Early Sciatica Symptoms You Shouldn’t Ignore
Radiating Pain Down One Leg
One of the most recognizable sciatica symptoms is pain that travels from the lower back or buttock down the leg. Unlike general back pain, sciatic pain follows a nerve pathway and often extends below the knee.
People frequently describe the sensation as sharp, electric, or burning. The pain may appear suddenly after lifting something heavy or twisting the spine, or it may develop gradually as spinal structures begin pressing on the nerve.
Activities such as sitting for long periods, coughing, sneezing, or bending forward often intensify the pain. Walking or changing position may temporarily relieve discomfort, but the nerve irritation typically returns.
Numbness and Tingling in the Leg or Foot
Another common early warning sign involves abnormal sensations along the nerve pathway. People may feel tingling, “pins and needles,” or patches of numbness in the leg, calf, or foot.
These sensations occur when nerve signals are disrupted by compression or inflammation. The affected area often matches the path of the irritated nerve root. For example, numbness near the top of the foot may indicate irritation of the L5 nerve root.
Although occasional tingling may seem minor, persistent numbness signals that the nerve is under pressure and should be evaluated by a specialist.
Muscle Weakness in the Leg
Sciatica doesn’t only affect sensation. It can also interfere with the muscles controlled by the sciatic nerve.
As compression worsens, muscle weakness may develop in the leg or foot. Some people notice difficulty lifting the front of the foot while walking, a condition often referred to as foot drop. Others may struggle to stand on their toes or push off the ground while walking.
Weakness indicates that the nerve is not sending strong signals to the muscles. When this occurs, early medical assessment becomes especially important to prevent permanent nerve damage.
Pain That Worsens With Sitting
Many patients with early sciatica notice that symptoms intensify when sitting for long periods. Sitting increases pressure on the lumbar discs and surrounding tissues, which can aggravate nerve compression.
Office workers, drivers, and individuals with sedentary lifestyles often experience this pattern. Pain may ease when standing or walking, only to return again when sitting.
Recognizing this pattern helps distinguish sciatica from other types of back discomfort.
What Causes Sciatica Symptoms?
Several structural conditions in the spine can irritate or compress the sciatic nerve. Understanding these causes helps explain why symptoms appear and how they progress.
Herniated Lumbar Disc
A herniated disc is one of the most frequent causes of sciatica. Spinal discs act as cushions between vertebrae. When the soft inner material pushes through the outer layer, it may press directly on a nerve root.
This compression often occurs in the lower spine at the L4-L5 or L5-S1 levels. When a disc presses against the nerve root, pain and neurological symptoms can travel down the leg along the sciatic nerve.
Disc herniation often follows lifting injuries, sudden twisting movements, or repetitive strain on the lower back.
Lumbar Spinal Stenosis
Another common cause is lumbar spinal stenosis, a condition where the spinal canal narrows and reduces space for nerves.
As the spine ages, discs lose height and joints may develop arthritis. These changes can lead to thickened ligaments and bone growth that crowd the spinal canal.
This narrowing places pressure on the nerve roots and can produce classic sciatica symptoms, particularly leg pain that worsens during walking or standing.
Bone Spurs and Degenerative Changes
With age, the spine undergoes natural wear and tear. As cartilage breaks down, the body may develop small bone growths called osteophytes, commonly known as bone spurs.
These spurs can narrow the openings where nerves exit the spine. Over time, this pressure irritates nerve roots and contributes to sciatica.
Degenerative disc disease and arthritis frequently contribute to these structural changes.
Piriformis Syndrome
In some cases, the sciatic nerve becomes irritated outside the spine. The piriformis muscle, located deep in the buttock, sits close to the sciatic nerve.
When this muscle tightens or spasms, it can compress the nerve and create pain that mimics traditional sciatica. Athletes, runners, and individuals who sit for extended periods may develop this condition.
Lifestyle and Health Factors That Increase Risk
Certain habits and health conditions make sciatic nerve irritation more likely.
Excess body weight increases stress on the lumbar spine and accelerates disc degeneration. Sedentary lifestyles weaken the core muscles that support spinal alignment.
Occupations that involve heavy lifting, bending, or prolonged sitting also place significant strain on the lower back. Construction workers, nurses, drivers, and office professionals may all experience higher risk.
Smoking reduces blood flow to spinal tissues, accelerating disc damage and slowing healing. Chronic health conditions such as diabetes can also make nerves more vulnerable to injury.
Maintaining a healthy weight, strengthening core muscles, and practicing proper lifting techniques can reduce the likelihood of developing sciatica.
Warning Signs That Require Immediate Medical Attention
Most cases of sciatica improve with conservative treatment. However, certain symptoms suggest serious nerve compression that requires urgent medical care.
Severe or rapidly worsening leg weakness may indicate significant nerve damage. When a person suddenly struggles to walk or control leg movement, immediate evaluation is necessary.
Another emergency condition is Cauda Equina Syndrome, a rare but serious disorder caused by intense compression of the nerve roots at the base of the spine.
Key warning signs include loss of bladder or bowel control, numbness around the groin or inner thighs, and rapidly worsening leg weakness. Emergency surgery is often required to relieve pressure on the nerves and prevent permanent damage.
Persistent back pain accompanied by fever, unexplained weight loss, or a history of cancer also requires prompt medical investigation.
How Doctors Diagnose Sciatica
Diagnosing sciatica begins with a thorough medical history and physical examination. Physicians evaluate pain patterns, muscle strength, reflexes, and sensory changes in the leg.
One common test is the straight leg raise. During this test, the doctor gently lifts the patient’s leg while lying flat. If pain shoots down the leg during the movement, it often suggests nerve root irritation.
Imaging studies may be recommended when symptoms persist or when severe neurological signs appear. Magnetic resonance imaging provides detailed images of discs, nerves, and spinal structures, helping identify the source of compression.
In some cases, nerve conduction studies or electromyography may be used to assess how well electrical signals travel through the nerve.
Early diagnosis helps guide treatment and prevents further nerve damage.
Treatment Options for Sciatica Symptoms
Treatment depends on the severity and cause of nerve compression.
Most cases improve with conservative care. Rest, physical therapy, and anti-inflammatory medications often reduce pain and inflammation. Gentle exercises help strengthen the core muscles and improve spinal stability.
Targeted stretching programs can relieve tension around the nerve. Physical therapists frequently recommend hamstring stretches, piriformis stretches, and lumbar mobility exercises to reduce pressure on the sciatic nerve.
If symptoms persist, doctors may recommend corticosteroid injections to reduce inflammation around the nerve root. These injections can provide temporary relief while allowing patients to continue rehabilitation exercises.
Surgery is usually reserved for cases where nerve compression causes severe pain, progressive weakness, or loss of bladder or bowel control.
Experienced orthopedic surgeons, including specialists like Dr. Gerardo Mangino, carefully evaluate each patient to determine whether surgical treatment is necessary or if conservative care will provide relief.
Preventing Future Sciatica Episodes
Although not all cases are preventable, certain habits can protect the spine and reduce the likelihood of recurring nerve pain.
Mantener los músculos centrales fuertes apoya la parte inferior de la espalda y reduce la tensión en los discos espinales. La actividad física regular también mejora la flexibilidad y la circulación en los tejidos de la columna vertebral.
Las técnicas de levantamiento adecuadas desempeñan un papel importante en la prevención. Levantar objetos con las piernas en lugar de hacerlo con la espalda ayuda a evitar levantamientos repentinos lesiones discales.
La postura también importa. Sentarse con el soporte lumbar adecuado y hacer pausas frecuentes para hacer movimientos puede reducir la presión en la columna vertebral durante las largas jornadas de trabajo.
Estos cambios simples a menudo marcan una diferencia significativa a la hora de prevenir el futuro síntomas de ciática.
Preguntas frecuentes
¿Cuáles son los primeros síntomas de la ciática?
El más temprano síntomas de ciática a menudo incluyen dolor en la parte baja de la espalda que desciende por una pierna. Muchas personas notan hormigueo, ardor o entumecimiento a lo largo de la trayectoria del nervio ciático. Estas sensaciones pueden empeorar al sentarse, toser o agacharse hacia adelante.
¿Cuánto suelen durar los síntomas de la ciática?
La ciática aguda generalmente mejora en varias semanas con reposo y tratamiento conservador. Sin embargo, los síntomas que duran más de ocho semanas pueden indicar una compresión nerviosa crónica y deben ser evaluados por un profesional médico.
¿La ciática puede desaparecer por sí sola?
Sí, muchos casos leves mejoran con el tiempo, el movimiento y los medicamentos antiinflamatorios. Sin embargo, no se deben ignorar el dolor, el entumecimiento o la debilidad persistentes, ya que pueden indicar una compresión nerviosa significativa.
¿Qué actividades se deben evitar con la ciática?
Las actividades que implican levantar objetos pesados, torcer la columna vertebral o estar sentado durante mucho tiempo pueden empeorar síntomas de ciática. Caminar suavemente y hacer ejercicios de estiramiento guiados suelen ser más seguros y pueden ayudar a aliviar la presión sobre el nervio.
Dé el primer paso hacia un movimiento sin dolor
Vivir con un dolor nervioso persistente puede resultar agotador. Las sacudidas bruscas, las sensaciones de hormigueo y la debilidad muscular causadas por síntomas de ciática puede interferir con el sueño, el trabajo y las actividades que le gustan. Sin embargo, ignorar las señales de advertencia con frecuencia permite que el problema empeore con el tiempo.
La evaluación temprana y el tratamiento personalizado pueden marcar una diferencia significativa. Especialistas como Dr. Gerardo Mangino se centran en identificar la causa raíz del dolor nervioso y en brindar atención ortopédica avanzada diseñada para restaurar la movilidad y la comodidad.
Si has notado dolor, entumecimiento o debilidad persistentes en las piernas, puede que sea el momento de buscar la orientación de un experto. Con el diagnóstico y el plan de tratamiento correctos, puedes recuperar la confianza en el movimiento y volver a una vida activa y sin dolor.
Su camino hacia el alivio puede comenzar con una simple consulta.


.png)
.png)
.jpg)




